by Good Health Centre | Apr 7, 2018
With a variety of literature festivals coming up, we’ve asked our staff about their favourite books … Receptionist Linda H – ‘Famous Five’ by Enid Blyton. “As a child I had many adventures and always wanted to be part of the famous five.” Receptionist Linda P –...

by Good Health Centre | Apr 7, 2018
‘Stress is an important dragon to slay – or at least tame – in your life.’ (Marilu Henner) People have different ideas of what stress is or feels like, but the majority of us would say we have experienced stress at some point in our lives. We consider stress to be...

by Good Health Centre | Apr 7, 2018
A marathon … a race which London Marathon co-founder Chris Brasher called ‘The World’s Most Human Race’. Thousands of people enter the London Marathon each year, and we can see why. There’s a buzzing atmosphere, and spectators showcase the best of the human spirit, as...

by Good Health Centre | Apr 7, 2018
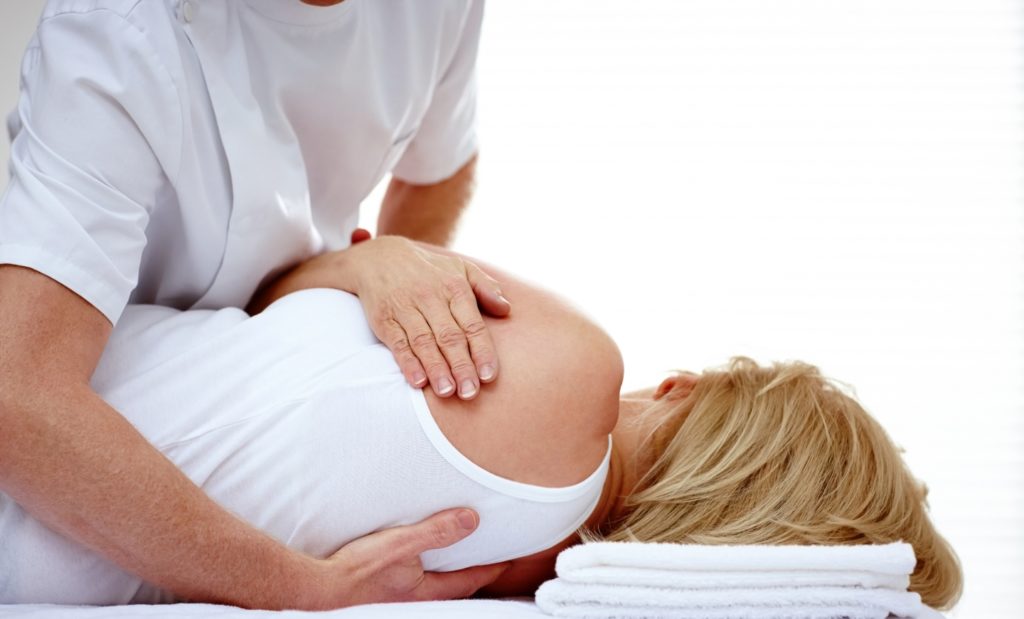
This quarter we are looking at the Piriformis muscle, and how it can affect the sciatic nerve. Piriformis Piriformis (meaning pear-shaped) is a muscle in the gluteal region of the lower limb. It is one of the six muscles that laterally (to the side) rotate the hip....

by Good Health Centre | Apr 7, 2018
This quarter brings both MS Awareness week, running from 23rd – 29th April, and World MS Day on 30th May. MS – the basics A neurological condition that affects the nerves in the brain and spinal cord. The word ‘sclerosis’ means scarring or hardening of small patches...






Recent Comments